But health and safety questions must be addressed
By Dorothy Wigmore
Asking questions is important these days. Many deal with pandemic health and safety issues for education staff and students. Who answers the questions matters. For education staff, school nurses and health and safety specialists are key sources.
“We can provide vaccine confidence, the evidence, the right information, and help people who are hesitant by promoting school nurses who are getting vaccines,” says Robin Cogan, Legislative co-chair for the New Jersey State School Nurses Association (NJSSNA). “We’re the medical interpreters.”
Messaging is important.
“It’s so important that it comes from members of a community,” Cogan says. “From a public health standpoint, we have to do a good job as the credible folks in our community. For schools, that’s what school nurses are—we’re trusted. People look to us for information. We can translate information. It’s been confusing. There’ve been lots of changes and the CDC has constant updates. Now, thankfully, with a new director, the CDC’s reviewing the prior messaging and revising it.”
The federal Occupational Safety and Health Administration (OSHA) also is changing its COVID requirements. President Joe Biden has appointed a new deputy assistant for pandemic and emergency response at OSHA. His responsibilities include a possible emergency temporary standard about pandemic health and safety by March 15. It would apply to all workplaces, including schools.
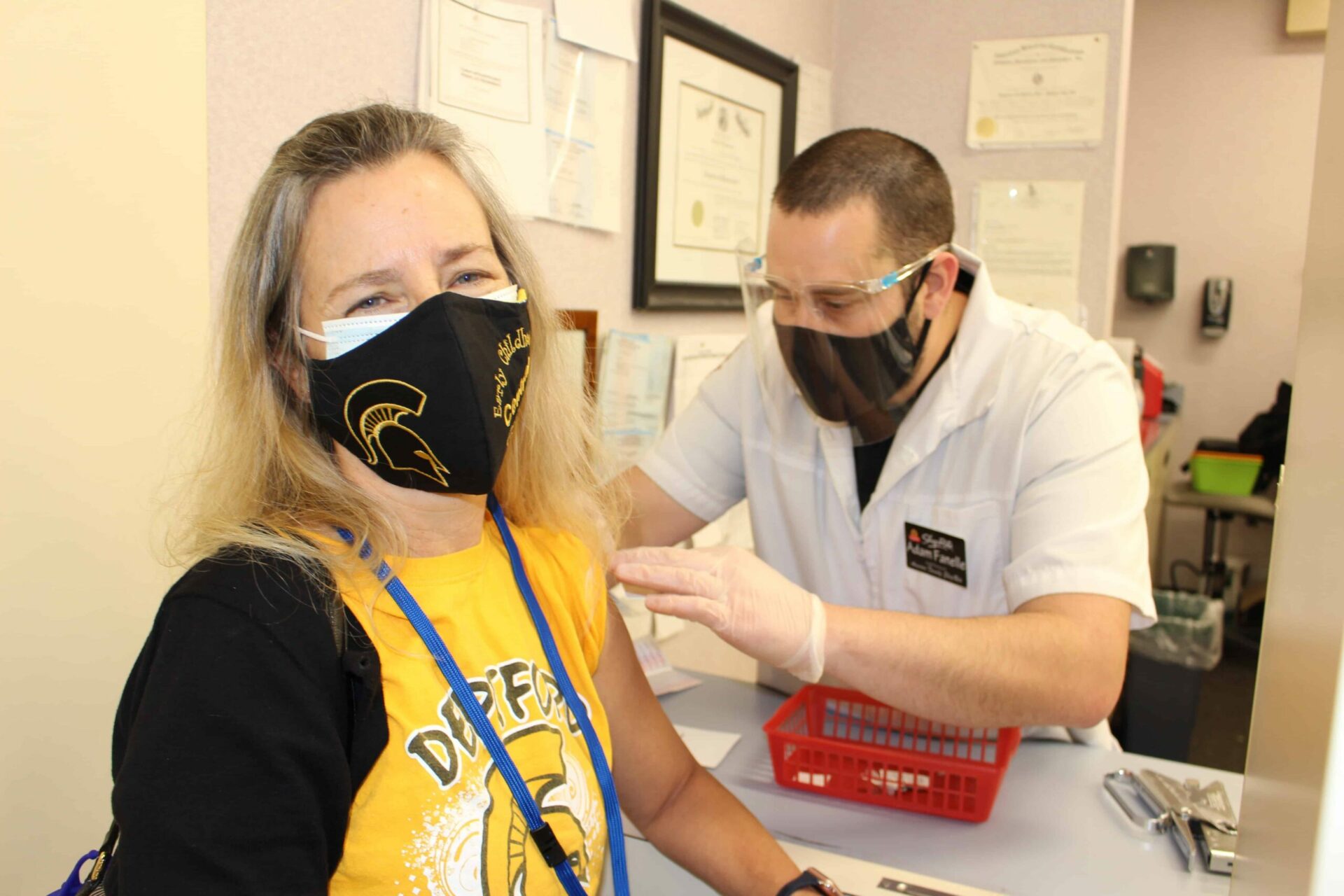
Vaccine confidence
There are questions about the vaccines themselves, the roll-out process, and the health and safety issues that go with giving them. NJEA has a FAQ (see references). So how can school nurses respond to questions?
“I try my best to share the importance of protecting ourselves,” Cogan says. “A typical vaccine is not 95% effective, like the Moderna and Pfizer vaccines. That’s quite amazing. Our children now are protected from 14 childhood illnesses because of vaccines. We have to remind people how vaccines have changed the world and kept us from so much harm.”
Eileen Gavin, the other NJSSNA Legislative co-chair, likes the term “generational amnesia.”
“Some people—many of them younger—say they’ll wait for FDA approval,” says Gavin. “They didn’t have the experience of classmates paralyzed with polio, in iron lungs, so they really don’t understand the history of vaccines and how many diseases they’d eradicated. They don’t have that generational confidence. I do because I saw the wreckage in many families from vaccine preventable diseases.”
“The stars aligned so the vaccines could come out quickly, but the science isn’t new,” Gavin says. “And they’re approved as an emergency measure because we need them now. For those concerned about the mRNA versions, others are expected to be available.”
“We’re asked about adverse reactions,” she added. “So we share experiences about the normal reactions to the vaccines like the flu shot, role-modeling and building vaccine confidence. We say it’s well worth it because of the devastation of COVID—500,000 US deaths, they’re saying, by mid-February.”
Like Gavin, school nurses can be recruited to be vaccinators. If they do that in school buildings—which may happen to increase access with vaccines that don’t need special refrigeration—others, such as custodial staff, also will be needed.
Vaccinators need health and safety protections
“Occupational health specialists want to ensure that those giving vaccinations, and people working with them, are properly trained and protected,” says Allen Barkkume, an industrial hygiene consultant with the New Jersey Work Environment Council (NJWEC).
“Vaccinators need respirators, such as N95s that filter and fit, in case someone is infected with something. PEOSH’s [Public Employees Occupational Safety and Health] respirator standard requires employers have effective programs, with medical evaluations, fit testing, training. etc.”
“Don’t forget the bloodborne pathogens (BBP) standard also requires safe needles to avoid needlestick injuries,” Barkkume adds.
Under state law, if workers might encounter blood or other bodily fluids, employers must have a BBP program to avoid needlestick injuries that can lead to bloodborne diseases like hepatitis and HIV. Employers must provide training, reporting processes and record needlestick injuries on their NJOSH–300 work-related injuries and illnesses log.
Safe devices have a covering designed to ensure no one gets stabbed by a syringe needle. Combined with a sharps container for disposal, they also protect those cleaning up after others use needles.
“Safe needles can be more awkward to use,” Gavin says. “Still, it’s not right to avoid using the shield. They’re expecting vaccinators to do things quickly and a lot of retired people are involved, who aren’t used to this. They need the safe needle training.”
“Just because someone doesn’t have COVID, it doesn’t mean they don’t have hepatitis or something else that spreads through blood. Vaccine sites need to have universal precautions,” Barkkume says.
If school nurses are giving the vaccine, Barkkume says they need to be familiar with whatever they’re using, and have the time to use and dispose of it properly. They also need easy access to hand-washing facilities and extra sharps boxes.
“If it’s happening in a makeshift arrangement, the vaccinator needs to know their way around and have stable surfaces to work on. And there’s no using your second hand to recap the needle.”
Barkkume recommends health and safety committees work with school nurses to ensure all staff involved with school site vaccinations are properly protected.
“They can encourage people getting the vaccine to be patient, so there’s less chance of needlestick injuries,” he says. “They also can remind members that we still need to distance and wear face coverings, even if you’ve had the vaccine.”
“It’s the kind of solidarity we need these days.”
Dorothy Wigmore is a long-time health and safety specialist, trained in occupational hygiene, ergonomics and “stress.” A Canadian, she also has worked in the U.S. and Mozambique, focusing on prevention and worker participation to solve job-related hazards.
Resources
NJEA Vaccine FAQ
njea.org/njea-vaccine-faq
National Institute of Environmental Health Sciences (NIEHS), “COVID-19 Vaccine Information for Workers”
bit.ly/nihc19vac
National Institute of Environmental Health Sciences (NIEHS), “Injection Safety for COVID-19 Vaccinators and Vaccine Administrators Preventing Needlesticks and Blood Exposures”
bit.ly/nihinjectionsafety
PBS, “3 things you should know about coronavirus vaccines”
bit.ly/pbsc19vac
PEOSH Revised Bloodborne Pathogens Standard
bit.ly/peoshbps
PEOSH respiratory protection standard
bit.ly/peoshrps